Bed-wetting: Practical Help for Kids and Adults
Bed-wetting is common and embarrassing, but it’s often fixable. Whether it’s a child who still wets the bed or an adult with new problems, small changes can make a big difference. This page gives practical steps you can try tonight, clear signs to see a doctor, and simple medical options that actually work.
Simple daily steps that help
Start with a routine. Cut down evening drinks an hour before bed and make sure the last bathroom visit is right before lights-out. Encourage regular daytime bathroom breaks every 2–3 hours so the bladder gets used to holding urine.
Constipation makes bed-wetting worse. Check for hard stools or less frequent poops. If bowel habits are off, fixing them often reduces accidents at night.
Use a reward chart for kids. Positive reinforcement works better than shaming. Celebrate dry nights with a sticker or small treat. For teenagers and adults, set realistic goals—track progress and reduce pressure on yourself.
Protect bedding to reduce stress. A waterproof mattress cover and washable sheets take the worry out of accidents and help everyone sleep more calmly.
Tools and medical options
Bedwetting alarms are very effective for many children. The alarm senses wetness and wakes the sleeper to finish in the bathroom. It takes patience, but alarms retrain the brain to respond to bladder signals.
There are also short-term medicines. Desmopressin (DDAVP) reduces urine at night and can help with sleepovers or trips. Talk to your doctor about dosing and safety—don’t buy medicine without a prescription. Anticholinergic drugs may help if the bladder is overactive, but they have side effects, so use them under medical advice.
If bed-wetting starts suddenly in an older child or adult, look for causes: urinary tract infections, diabetes, changes in sleep, certain medications, or obstructive sleep apnea. A simple urine test and a medical check can rule out serious problems.
Behavioral therapy helps too. Bladder training exercises and timed voiding strengthen control. For children, motivational support from parents and teachers reduces anxiety and improves results.
When to call a doctor? If accidents start suddenly, come with pain, burning, fever, blood in urine, or increased thirst and weight loss, see a clinician quickly. Also consult a doctor if bed-wetting continues past age 7–8 or if it affects the child’s emotional life or school.
Want to try a plan? Start with a one-week checklist: limit drinks before bed, schedule a bathroom visit at lights-out, use protection on the mattress, and record nights. If there’s no improvement after a month or if you see warning signs, book a medical visit.
Bed-wetting isn’t a personal failure. With steady steps, most kids and many adults see big improvements. Small routine changes, the right tools, and medical advice when needed usually do the job.
Understanding the role of the kidneys in bed-wetting
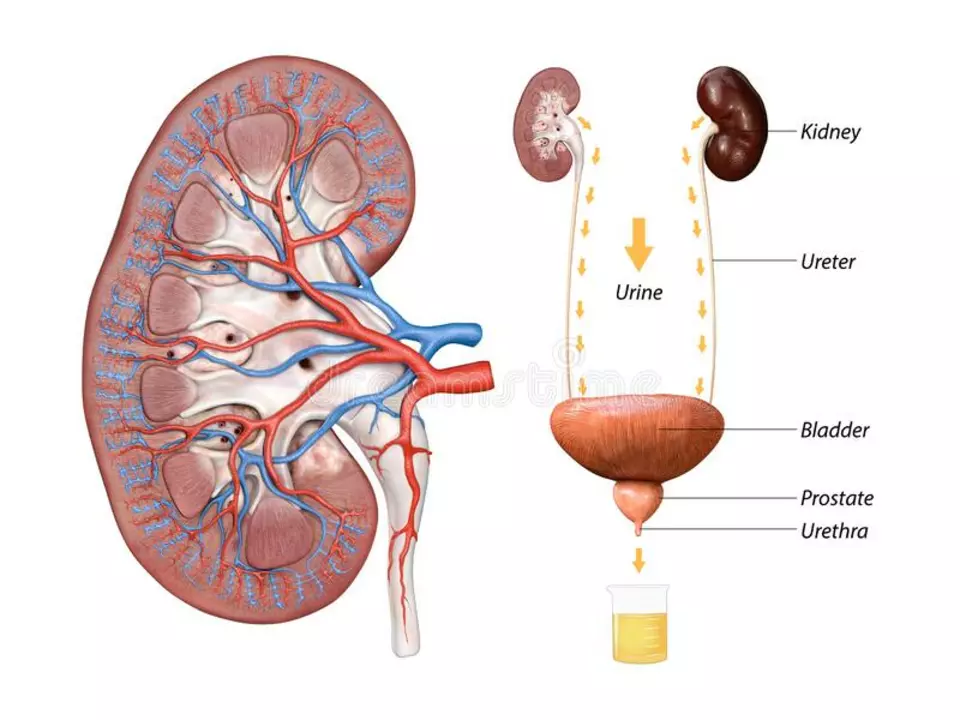
As a blogger who recently researched the topic of bed-wetting, I have gained a deeper understanding of the role kidneys play in this condition. It turns out that our kidneys are responsible for filtering waste from our blood and producing urine, which is then stored in the bladder. Bed-wetting, or nocturnal enuresis, can occur when the kidneys produce too much urine during sleep or when the bladder muscles are unable to hold the urine. Additionally, hormones that regulate urine production may be imbalanced, leading to excessive production at night. It's important to remember that bed-wetting is a common issue, especially among children, and understanding the role of the kidneys can help us find effective solutions.
Read More