When a vertebra collapses due to osteoporosis, trauma, or cancer, the pain can be crushing - literally. Many people describe it as a constant, deep ache that makes standing, sitting, or even breathing painful. For years, the only options were bed rest, painkillers, or risky open surgery. But today, two minimally invasive procedures - kyphoplasty and vertebroplasty - are helping tens of thousands of people get back on their feet in hours, not months.
How These Procedures Work
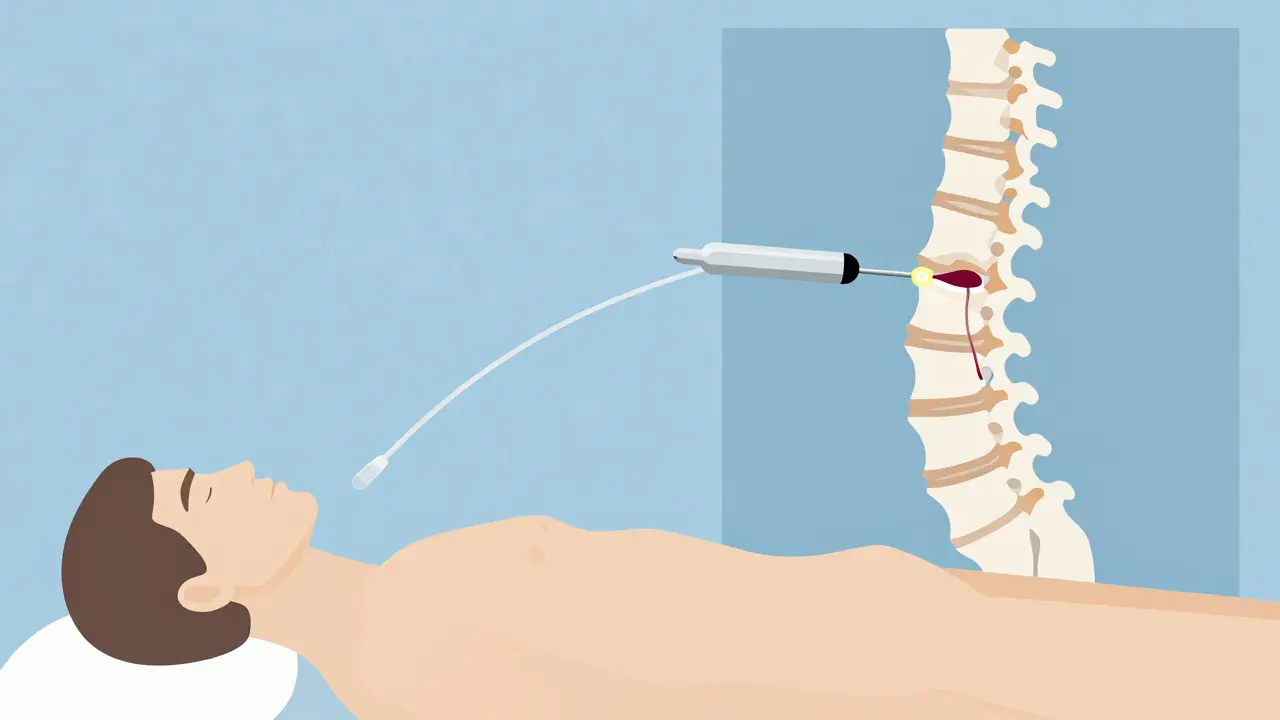
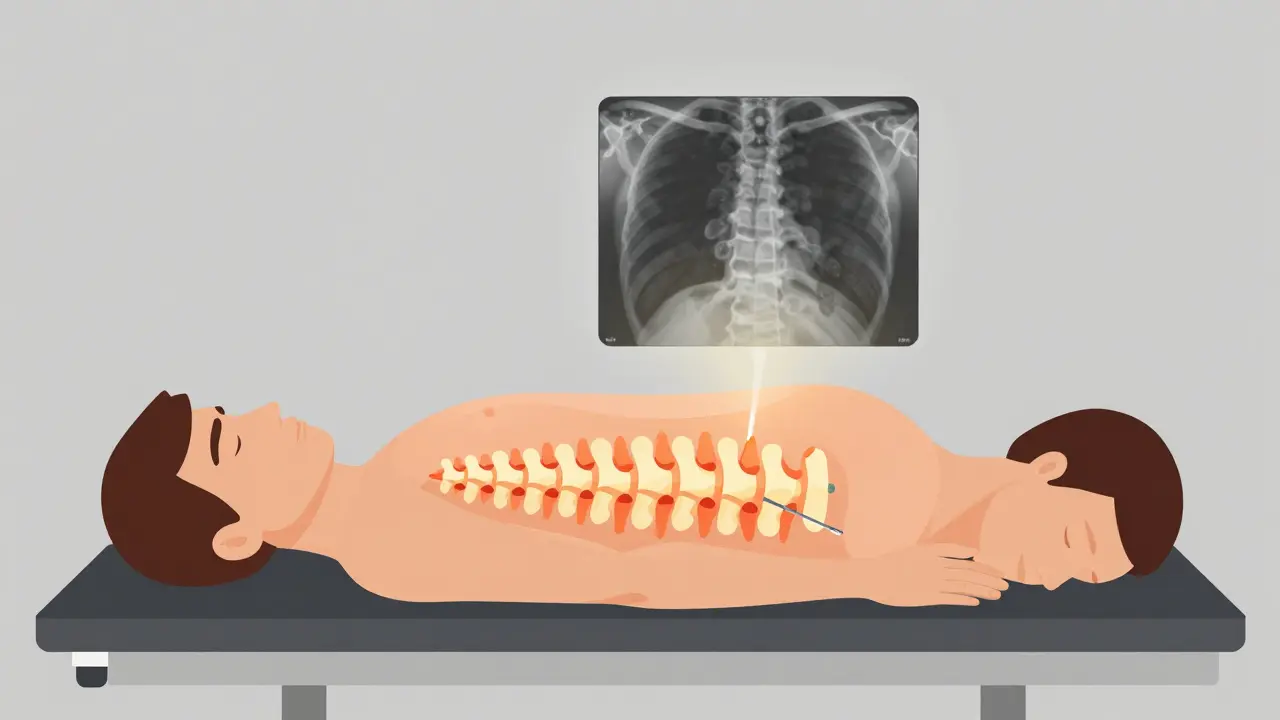
Both kyphoplasty and vertebroplasty fix broken spinal bones using medical-grade bone cement. The goal isn’t to rebuild the entire spine, but to stabilize the fractured vertebra, stop the pain, and let you move again. The whole process takes about 30 to 60 minutes, usually done with local anesthesia and light sedation. You’re awake but relaxed, lying face down on the table while a specialist uses real-time X-ray imaging to guide the procedure.In vertebroplasty, a thin needle is inserted through the skin and into the fractured bone. Then, liquid cement - called polymethylmethacrylate (PMMA) - is injected directly into the damaged area. The cement hardens in 10 to 20 minutes, locking the broken pieces together like a cast. It’s simple, fast, and effective.
Kyphoplasty adds a step before the cement goes in. A small balloon is inserted through the same needle and gently inflated inside the fractured bone. This balloon creates a cavity and, in many cases, lifts the collapsed vertebra back toward its normal height. Once the balloon is deflated and removed, the cement is injected into the space it left behind. This extra step gives kyphoplasty its name - from the Greek word kyphos, meaning hunchback.
Key Differences Between the Two
The biggest difference isn’t just technique - it’s what each procedure can do for your spine’s shape.
Vertebroplasty fixes the pain but doesn’t change the spine’s structure. If you had a collapsed vertebra that made you look hunched, vertebroplasty won’t fix that. The cement just fills the crack. Studies show it restores less than 5% of lost height on average.
Kyphoplasty, on the other hand, can restore 40% to 60% of the original height of the fractured bone. That’s not just cosmetic - it helps improve posture, reduces pressure on nearby nerves, and can make breathing easier. But here’s the catch: that height gain doesn’t always last. A 2007 study in Spine found that after just 500 normal spinal loads (like walking or standing), the restored height dropped by about 30%. So while kyphoplasty gives you better shape right away, the long-term structural benefit isn’t as strong as once thought.
Which One Is Safer?
Safety matters. Both procedures are generally low-risk, but complications do happen.
The biggest risk with both is cement leaking out of the bone. In vertebroplasty, this happens in 27% to 68% of cases. Most leaks are harmless and cause no symptoms. But in about 1.1% of vertebroplasty cases, the cement leaks into the spinal canal or blood vessels - which can lead to serious problems like nerve damage or lung blockage.
Kyphoplasty cuts that risk in half. Because the balloon creates a controlled space for the cement, the injection pressure is lower and the cement flows more predictably. Cement leakage happens in only 9% to 33% of kyphoplasty cases. Symptomatic leaks - the kind that cause real problems - occur in just 0.6% of patients, compared to 1.1% for vertebroplasty.
Both procedures carry a small risk of new fractures in nearby vertebrae. About 5% to 10% of patients develop another fracture within a year. This isn’t because the procedure caused it - it’s because osteoporosis is still active. The bone around the treated area is still weak. That’s why treating the root cause - osteoporosis - is just as important as the procedure itself.
Pain Relief: Do They Work?
If you’re wondering whether these procedures actually stop the pain - yes, they do. And they do it fast.
Studies show that 85% to 90% of patients experience major pain relief within 24 hours. On a scale of 1 to 10, average pain scores drop from 8.2 before the procedure to 1.5 after. Many patients say it feels like a switch was flipped.
There’s almost no difference in pain relief between kyphoplasty and vertebroplasty. Both work equally well at stopping pain. That’s why many experts argue that if you don’t need height restoration, vertebroplasty is just as good.
Patients on platforms like Healthgrades give kyphoplasty a 4.6/5 rating and vertebroplasty a 4.4/5. One patient on Reddit said, “I went from 9/10 pain to 2/10 within hours.” Another said, “My pain dropped, but I still look hunched.” That’s the difference.
Cost and Accessibility
Kyphoplasty costs 20% to 30% more than vertebroplasty. In the U.S., Medicare pays about $3,850 for kyphoplasty and $2,950 for vertebroplasty. The price difference comes from the balloon device - it’s a specialized tool that adds to the cost.
But cost isn’t just about the procedure. Kyphoplasty usually requires more training, more time in the operating room, and more equipment. That’s why many hospitals offer both, but choose based on the patient’s needs.
Insurance - including Medicare - covers both procedures if you’ve tried conservative treatments first. That means at least 4 to 6 weeks of pain medication, physical therapy, or a back brace without improvement. If your MRI shows fresh bone swelling (bone marrow edema), you’re likely a candidate.
Who Gets Which Procedure?
It’s not one-size-fits-all. Your doctor will consider three things: fracture type, pain level, and bone condition.
- If your fracture is recent, painful, and the bone has collapsed more than 30%, kyphoplasty is often preferred. It gives you the best shot at restoring posture and reducing long-term deformity.
- If the fracture is stable, the bone hasn’t lost much height, and you’re mostly dealing with pain, vertebroplasty is just as effective - and cheaper.
- If you have weak bone quality (severe osteoporosis), kyphoplasty’s controlled cavity may lower the risk of cement leakage.
Dr. Richard Jensen, a spine expert at Oregon Health & Science University, says: “For most patients without major deformity, vertebroplasty gives the same pain relief at a lower cost. That’s better value.”
But Dr. John Kallmes, who helped invent kyphoplasty, adds: “The balloon doesn’t just make the procedure safer - it gives us more control. That matters when bone is fragile.”
Recovery and Aftercare
You’ll go home the same day. Most people walk within a few hours. You’ll need to avoid heavy lifting for 24 hours, then slowly return to normal activity over the next week.
Here’s what most patients report:
- 92% return to daily activities within 72 hours
- 75% stop using opioids within one week
- Most stop wearing back braces within a month
But recovery isn’t just about the procedure. Osteoporosis doesn’t go away. If you don’t treat it, you’re at high risk for another fracture. That means:
- Bone-strengthening medications like bisphosphonates or denosumab
- Calcium and vitamin D supplements
- Balance training to prevent falls
Without these, even the best procedure won’t stop the next fracture.
What’s New in 2026?
The field is evolving. In 2023, Medtronic got FDA approval for a new calcium phosphate cement that hardens slower and feels more like natural bone. It’s less likely to overheat during hardening, which reduces tissue damage.
A major 2023 study in The Lancet found that patients who got either procedure within two weeks of their fracture had a 28% lower risk of dying within a year compared to those who only got pain meds. That’s huge. It suggests these aren’t just pain treatments - they’re life-saving.
Right now, a large trial called COAST is comparing kyphoplasty and vertebroplasty over two years to see if height restoration actually leads to better mobility, less back pain, or fewer future fractures. Results are expected late 2024.
Market analysts predict kyphoplasty will make up 75% of all vertebral procedures by 2028 - not because it’s better at pain relief, but because it’s safer and fits better with modern expectations of care.
Final Thoughts
Both kyphoplasty and vertebroplasty are life-changing for people with painful spinal fractures. They’re not magic, but they’re close. If you’re tired of living with constant pain, unable to stand without help, or afraid to move - these procedures offer real hope.
Don’t choose based on hype. Choose based on your fracture, your body, and your goals. If you’re mostly in pain and don’t care about posture, vertebroplasty is fast, cheap, and effective. If you’ve lost height, have a severe hunch, or have fragile bones, kyphoplasty gives you a better chance at restoring function.
Either way, you’re not alone. Over 100,000 people in the U.S. alone get one of these procedures every year. And most of them - 9 out of 10 - say it was the best decision they made for their health in years.
Are kyphoplasty and vertebroplasty the same thing?
No. Both use bone cement to stabilize fractured vertebrae, but kyphoplasty adds a balloon step to restore height before injecting cement. Vertebroplasty injects cement directly without height restoration. Kyphoplasty is more complex and expensive, but may reduce cement leakage risk and improve posture.
Which procedure is better for osteoporosis-related fractures?
Both work well for osteoporosis fractures. If the bone has collapsed significantly (over 30% height loss), kyphoplasty is often preferred because it can restore some height and reduce deformity. If the fracture is stable with minimal collapse, vertebroplasty is just as effective at relieving pain - and costs less.
Do these procedures fix osteoporosis?
No. These procedures treat the fracture, not the underlying bone weakness. Osteoporosis must still be managed with medications, calcium, vitamin D, and fall prevention. Without treatment, you’re at high risk for another fracture.
How long does recovery take?
Most patients go home the same day. You can walk within hours. Avoid heavy lifting for 24 hours. Normal activities usually return within 1-2 weeks. Pain relief is often immediate - many report major improvement within 24 hours.
Is kyphoplasty worth the extra cost?
It depends. If you have major spinal deformity or fragile bone, kyphoplasty’s lower leakage risk and height restoration may justify the higher cost. If you’re mainly dealing with pain and no significant collapse, vertebroplasty offers the same pain relief at a lower price. Studies show no major difference in long-term pain outcomes.
Can these procedures be done more than once?
Yes. If another vertebra fractures later, either procedure can be repeated. Many patients get treated for multiple fractures over time, especially if osteoporosis isn’t well-controlled. Each procedure targets one fracture at a time.

bill cook
February 28, 2026 AT 04:49Katherine Farmer
March 1, 2026 AT 02:40Angel Wolfe
March 3, 2026 AT 01:56Vikas Meshram
March 3, 2026 AT 14:35Ben Estella
March 5, 2026 AT 13:59Jimmy Quilty
March 7, 2026 AT 09:48Miranda Anderson
March 8, 2026 AT 17:34Gigi Valdez
March 9, 2026 AT 01:43Sneha Mahapatra
March 10, 2026 AT 15:06Charity Hanson
March 11, 2026 AT 23:09Justin Ransburg
March 12, 2026 AT 07:51Sumit Mohan Saxena
March 12, 2026 AT 16:34Brandon Vasquez
March 13, 2026 AT 18:32Byron Duvall
March 14, 2026 AT 04:47