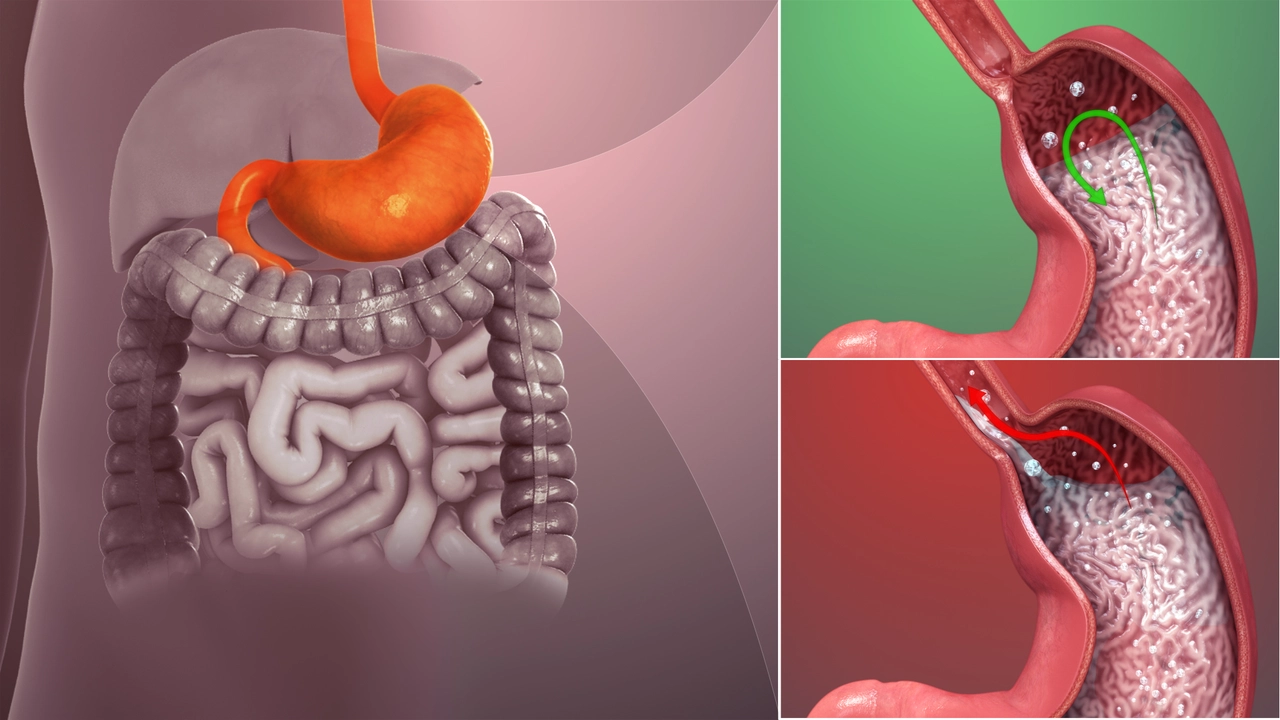
GERD (Acid Reflux): Clear Steps to Feel Better and Spend Less
Heartburn once in a while is normal. When it happens more than twice a week or starts affecting sleep, that’s GERD — gastroesophageal reflux disease. GERD means stomach acid keeps flowing back into your esophagus, causing pain, coughing, bad breath, or a sour taste. Left untreated, it can irritate or damage the lining of the esophagus.
Simple daily changes that cut reflux fast
Small changes often make a big difference. Try these first before reaching for stronger meds:
- Eat smaller meals and stop eating 2–3 hours before lying down. Big meals and bedtime snacks push acid up.
- Lose even a little weight if you’re overweight; belly fat raises stomach pressure.
- Raise the head of your bed 4–6 inches or use a wedge. Sleeping inclined keeps acid where it belongs.
- Avoid trigger foods: coffee, alcohol, chocolate, peppermint, spicy meals, fried or fatty foods, and citrus for some people. Keep a short food diary to spot your triggers.
- Quit smoking and avoid tight belts or waistbands that squeeze the stomach.
Medications and when to use them
If lifestyle changes aren’t enough, medicines can help. Antacids work fast for mild symptoms. H2 blockers (famotidine) lower acid for several hours and are cheap over the counter. Proton pump inhibitors (PPIs) like omeprazole or esomeprazole are stronger and used for more frequent or severe reflux. Take PPIs as directed — usually 4 weeks to see full benefit.
Long-term PPI use can have risks like low magnesium, bone loss, or infections in some people. Talk with a clinician about the lowest effective dose and whether you can step down to an H2 blocker or occasional antacid.
See a doctor right away if you have trouble swallowing, persistent vomiting, unexplained weight loss, coughing up blood, or black stools. Those are “alarm” signs and need evaluation. Tests can include an endoscopy or pH study to check acid and tissue damage.
Surgery and device options exist when meds fail or aren’t wanted. Fundoplication or newer devices like LINX can help, but they carry risks and need a specialist’s opinion.
How you manage GERD depends on symptom severity, health goals, and safety. Many people control reflux with modest lifestyle shifts plus occasional meds. Others need daily prescription therapy or procedural options — your doctor can guide the best path.
Want tips on saving money for meds or finding reliable pharmacies? Affordable options and safety checks are useful, but don’t skip proper prescriptions and licensed pharmacies when you need prescription drugs.
Quick take: try lifestyle fixes first, use the simplest medicine that works, watch for alarm signs, and talk with a clinician about long-term plans. Small, consistent steps usually bring the biggest relief.
Erosive Esophagitis and GERD: How They're Related and What to Do
In my recent research, I discovered the connection between erosive esophagitis and GERD (Gastroesophageal Reflux Disease). GERD is a common condition where stomach acid flows back into the esophagus, causing irritation and inflammation. This chronic exposure to stomach acid can lead to erosive esophagitis, which is a more severe form of esophageal damage. To prevent and manage these conditions, it's crucial to make lifestyle changes such as avoiding trigger foods, maintaining a healthy weight, and seeking medical advice for proper treatment. Remember, early intervention can help prevent long-term complications and improve overall quality of life.
Read More