Getting your prescription filled should be simple - but mistakes happen. A wrong dose, a mix-up in names, or a confusing label can lead to serious harm. In fact, medication errors are one of the leading causes of preventable harm in healthcare. The good news? You have the power to stop most of them before they start - just by checking your prescription label.
Every time you pick up a new prescription, take 30 seconds to verify five key things. It’s not just a good habit. It’s your last line of defense. And it works. Studies show that patients who check their labels reduce the chance of taking the wrong medication by 67%.
What Should Be on Your Prescription Label?
By law, your prescription label must include specific information. If any of these are missing or unclear, ask the pharmacist before leaving. Here’s what you should see:
- Your full legal name (first and last - sometimes middle initial too)
- The exact name of the medication (both brand and generic, if applicable)
- The strength (e.g., 5 mg, 10 mg, 500 mg - not just "a pill")
- The dosage form (tablet, capsule, liquid, patch)
- How much was dispensed (e.g., 30 tablets)
- Directions for use (e.g., "Take one tablet by mouth twice daily")
- The prescriber’s name
- The pharmacy’s name and phone number
- The date the prescription was filled
- The expiration date (if applicable)
- A National Drug Code (NDC) number - a unique 10- or 11-digit code
These aren’t suggestions. They’re federal requirements under FDA rules. If your label doesn’t include them, the pharmacy is out of compliance. Don’t be afraid to ask why something’s missing.
Step-by-Step: How to Verify Your Label
You don’t need a medical degree. You just need to slow down and look closely. Follow this simple 30-second routine every time you pick up a prescription:
- Hold the bottle at eye level. Good lighting matters. Natural daylight is best. If you’re in a dim pharmacy, ask to step near a window or turn on a light.
- Check your name. Does it match your government ID? Sometimes pharmacies use nicknames or misspellings. "John Smith" vs. "Jonathan Smith" - that’s a red flag. Even a missing middle initial can mean a different person.
- Match the medication name. Compare the label to what your doctor told you. If your doctor said "Lisinopril," but the label says "Zestril," that’s okay - Zestril is the brand name. But if it says "Lipitor," and you were prescribed for blood pressure, that’s wrong. Always check both brand and generic names.
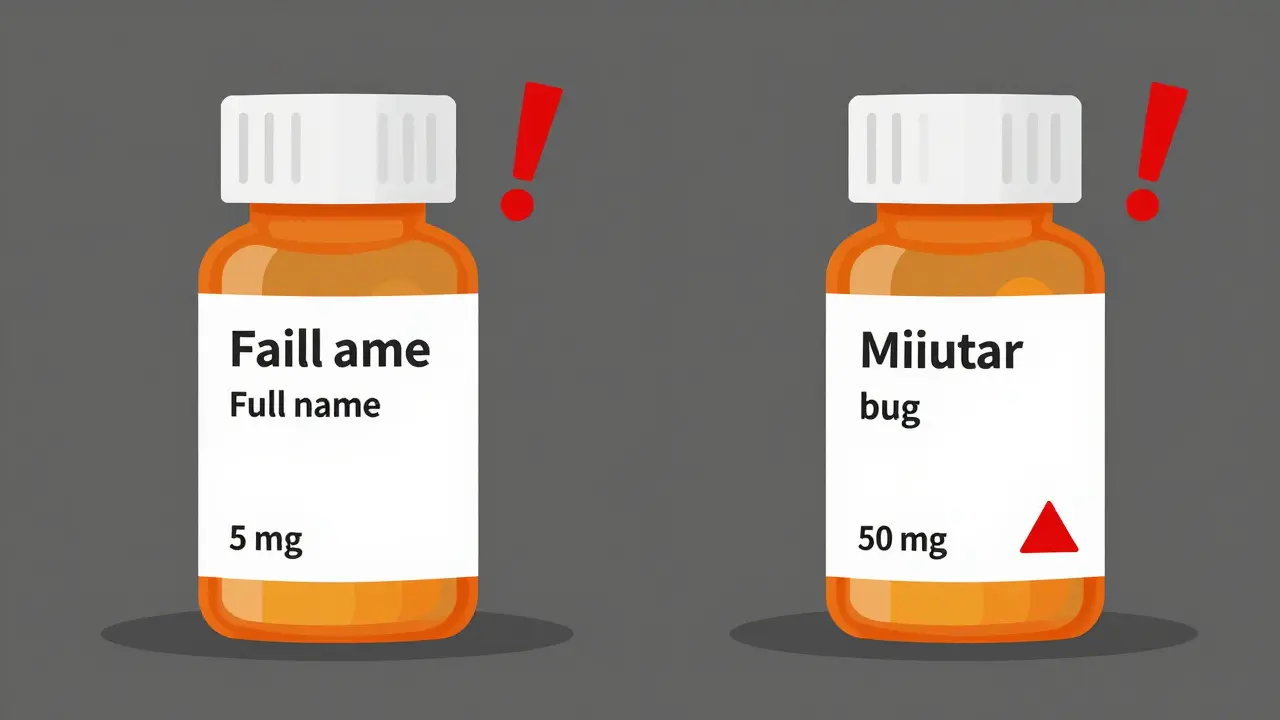
- Verify the strength. This is where most errors happen. A 5 mg pill and a 50 mg pill look similar. But 50 mg is ten times stronger. If your doctor said "5 mg," and the label says "50 mg," don’t take it. Call the pharmacy immediately.
- Confirm the directions. Did your doctor say "take once daily"? Does the label say "take twice daily"? Mismatches here can lead to overdose or under-treatment. If the directions are unclear, ask the pharmacist to explain them in plain language.
- Check the pharmacy contact info. If the phone number is smudged or missing, that’s a warning sign. Legitimate pharmacies always include this. It’s your lifeline if you have questions later.
That’s it. Six steps. Takes less than a minute. And it’s saved lives.
Common Mistakes and Real Stories
People don’t always catch errors. Here are real examples from patients who did - and didn’t:
- Caught in time: A woman in Texas picked up her mom’s blood thinner. The label said 10 mg. The doctor had prescribed 5 mg. She called the pharmacy. They had accidentally filled the wrong bottle. That mistake could have caused a life-threatening bleed.
- Almost missed: A man in Florida took his blood pressure pill and felt dizzy. He checked the label - his name was on it, but the pill looked different. He called the pharmacy. Turns out, his roommate’s prescription had been accidentally labeled with his name. He never took it.
- Too late: A 72-year-old woman in California took her diabetes pill and ended up in the hospital. The label said "Metformin 1000 mg" - but her doctor had prescribed 500 mg. She didn’t check the strength. The pharmacy had misread the handwriting.
These aren’t rare. A 2023 survey found that 18% of patients discovered an error on their prescription label in the past year. Most of those errors were caught by the patient - not the pharmacy.
What If You Can’t Read the Label?
Small print is a real problem. Over 37% of adults over 65 say they struggle to read prescription labels. The FDA recommends font sizes of at least 12-point for critical info. But many pharmacies still use 9-point or smaller.
Here’s what you can do:
- Ask for a large-print copy. Most pharmacies have them available.
- Use your smartphone camera. Zoom in. Turn on the flashlight. Most phones have a magnifier app built in.
- Carry a small pocket magnifier. They cost less than $10 and fit in your wallet.
- Ask the pharmacist to read it aloud while you watch.
- Request a printed copy with bigger text. Pharmacies are required to accommodate reasonable requests.
Also, if English isn’t your first language, ask for labeling in your native language. In states like California and New York, pharmacies must offer bilingual labels for the top five languages spoken in their area.
Why This Matters More Than You Think
Medication errors don’t just cause discomfort - they cause hospital stays, organ damage, and death. The Institute for Safe Medication Practices estimates that 1.5 million people are harmed every year in the U.S. because of mistakes like these. About a quarter of those errors come from labeling problems.
And here’s the truth: pharmacies aren’t trying to hurt you. They’re overworked. Pharmacists often fill 200+ prescriptions a day. A single misread handwriting, a mislabeled bottle, or a system glitch can slip through.
Your verification isn’t about blaming them. It’s about adding a safety net. Think of it like double-checking the seatbelt before driving. You don’t do it because you think the car is broken. You do it because you care about your safety.
Doctors and pharmacists agree. The American Medical Association now tells patients: "Always check your label." The FDA’s 2023 initiative specifically urges patients to verify five key elements. And states with mandatory verification counseling have seen 18% fewer errors.

What About Apps and Digital Tools?
There are apps like Medisafe and GoodRx that scan your label and remind you when to take pills. They’re helpful. But they’re not replacements.
Why? Because 98% of U.S. pharmacies still use paper labels. And 42% of prescription users are over 65 - many of whom don’t use smartphones for health tasks. Even if you use an app, you still need to look at the physical label. Apps can misread barcodes, lose connection, or fail to detect handwritten changes.
Think of apps as helpers - not replacements. Your eyes, your brain, and your willingness to ask questions are still the most reliable tools you have.
When to Call the Pharmacy
Don’t wait until you’ve taken the pill. If anything feels off - call right away. Here are the top reasons to call:
- Your name is wrong or incomplete
- The medication name doesn’t match what your doctor prescribed
- The strength is different (e.g., 5 mg vs. 50 mg)
- The directions say something your doctor didn’t
- The pill looks different from what you’re used to
- The label is faded, smudged, or hard to read
Pharmacists expect these calls. They’re trained to handle them. No one will judge you for asking. In fact, they’ll thank you.
Final Reminder: You’re the Last Line of Defense
Doctors write prescriptions. Pharmacists fill them. But you’re the one who takes them. That makes you the final checkpoint. No system is perfect. Technology fails. People make mistakes.
But you? You can stop it.
Next time you pick up a prescription, pause. Look. Read. Ask. It takes less than a minute. And it might save your life.





Andrew Poulin
March 7, 2026 AT 19:55Ferdinand Aton
March 8, 2026 AT 02:26amber carrillo
March 9, 2026 AT 07:57Aaron Pace
March 11, 2026 AT 03:42Adebayo Muhammad
March 12, 2026 AT 18:57Bridget Verwey
March 13, 2026 AT 02:23Weston Potgieter
March 15, 2026 AT 00:44Vikas Verma
March 16, 2026 AT 14:03